A recent paper published in Brain Communications has identified several lipid (fat-like) molecules that are elevated in MND, specifically amyotrophic lateral sclerosis (ALS) which is the most common form of MND. The study measured the levels of lipids in the blood of people living with ALS and how their lipid levels changed with time during their disease. This work looks to understand the impact of lipids in ALS and identify if they could be suitable as biomarkers for ALS. There is a great need to find biomarkers for ALS to help make quicker diagnoses and evaluate the effectiveness of potential treatments.
It has already been established that elevated levels of specific types of lipids are a common feature in ALS. However, there is a lack of understanding for how lipid levels change in ALS or in disease progression. More evidence is coming to light that shows that lipids are important factors in neurodegeneration. This further understanding is in part, due to improved methods of measuring levels and types of lipids in samples from people. These advances have allowed the detection of small, yet significant, changes in lipids that are critical to disease processes.
What are lipids?
Lipid is an umbrella term for fatty or waxy compounds in nature and are involved in numerous biological processes throughout the human body, making them an essential component for normal cellular functions. In the case of MND, the lipids cholesterol ester (ChE) and triglycerides (TG) have been suggested to be elevated in those living with MND, though the results from previous studies regarding the two have been inconsistent and contradictory.
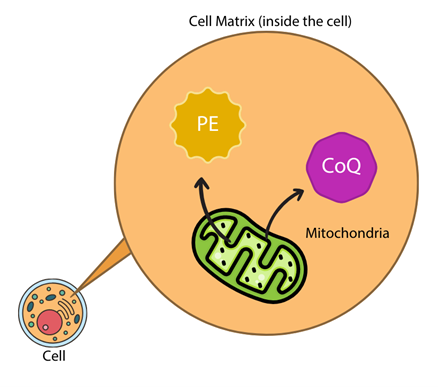
What are mitochondria and how are they involved in lipid production?
Mitochondria are organelles (the organs of the cells) that are involved in numerous biological pathways, but are most known for producing the energy molecules needed for biochemical reactions to take place. In terms of synthesising lipids, mitochondria are major producers of phosphatidylethanolamine (PE) and coenzyme Q10 (CoQ10), both of which are very important in mitochondrial processes.
What did this work focus on?
Previous studies were only able to measure a few types of lipids such as cholesterol and triglycerides at high levels, and could not provide an overall view of all types of lipids or differentiate individual types of lipids in blood. This limited the accuracy of analyses and certain lipid types may have been overlooked in terms of relevance to disease progression.
Recent technologies have allowed this study to measure all lipid types in the blood of those with ALS.
The two main aims of the project were:
- To identify the lipid pathways that were changed in ALS to understand what changes may lead to ALS.
- To identify lipids for potential biomarker development for ALS diagnosis and to monitor disease progression.
Which lipids did they investigate?
[tabs][tab title=”Phosphatidylethanolamine”] Is involved in maintaining the structure of mitochondria. Phosphatidylethanolamine is present at particularly high levels in the brain, nerves and spinal cord suggesting an important role in nervous system function.[/tab] [tab title=”Diglycerides”] Acts as a molecule that aids in biological signalling, allowing cells to communicate.[/tab][tab title=”Coenzyme Q10″] Is involved in the production of adenosine triphosphate (ATP) in a process known as electron transport chain in the mitochondria. ATP is known as energy currency and is essential in many biological processes.[/tab][tab title=”Acylcarnitine”] Is also involved in the production of ATP in the mitochondria in a process known as the Krebs cycle. [/tab][/tabs]What did the study uncover?
The researchers were interested in understanding the changes in lipid levels that occurred over time during disease and so analysed blood samples from people living with ALS and controls (people without ALS) over time. The study used multiple samples generously given by 28 people living with ALS and 22 controls.
A class of lipids known as diglycerides (DG) were found to have the highest levels of elevation in ALS blood compared to controls and this correlated to the concentration of neurofilament light chain (NfL). NfL is abundant in the axons of neurones and is found in increased amounts in the cerebrospinal fluid of those with neurological disorders. This suggests that an increase in diglycerides could indicate damage to neurones and therefore could be considered as a candidate biomarker for ALS.
Other lipid classes were reduced in ALS blood, including acylcarnitine (AcCa) and coenzyme Q8 (CoQ8), all of which are closely linked to processes in mitochondria. Levels of CoQ8 also correlated with NfL levels, meaning it could also be considered as a potential biomarker.
Several lipid classes which increased over time in controls, were found to decrease over the same time in ALS samples. One of them was phosphatidylethanolamine (PE) which they found was particularly associated with disease progression of ALS. This is a first as there was no known previous connection made between PE and ALS. Previous studies have indicated that PE is vital in maintaining working control of mitochondrial function and structure and have shown that removing the gene used to produce PE causes mitochondrial death. Mitochondria are essential for cell survival, so preventing (or correcting) the reduction in PE levels in people living with ALS, could be a potential therapeutic strategy.
RELATED TOPIC
Blog | 24 June 2022
Delving deeper into neurofilament light chain
What does this mean for people living with ALS?
Identifying elevated lipid levels in samples of people living with ALS highlighted several lipids that could potentially be used as biomarkers for disease progression. This could aid in quicker identification of ALS resulting in faster diagnosis so that treatment and care can begin earlier. Understanding the changes in lipid pathways will enable researchers to focus on affected mechanisms, potentially allowing for the development of new targeted therapies based on the changes in these pathways.
What are the next steps in this work?
The study pointed to multiple pathways of lipid changes in ALS. The findings support the idea that cellular changes in ALS involve precise changes in individual lipid pathways. Further studies will need to be conducted to fully understand the lipid pathways affected, the mechanisms involved and if changes in these affected pathways can be corrected.