Please note that this blog talks about sensitive topics such as death and tissue donation throughout.
Researchers use many different tools to increase our understanding of the underlying biology of the disease. These can be animal models of MND, biological samples from people with MND and brain tissue from people that have died from the disease. Using different methods to research the disease can highlight different things that might go wrong in MND and could contribute to the cause.
Dr Robin Highley works at the University of Sheffield and helps to manage a collection of brain tissue which researchers can use. We chatted to Robin about his work and the role it plays in helping to drive MND research forward.
Can you tell us a bit about yourself and the work that you do?
Why is neuropathology important?
Some of the most important treatments for age-related (neurodegenerative) brain disease come from neuropathology studies of tissue from real people with these diseases. Let me give two examples: Chemical analysis of the brains of people with Parkinson’s disease demonstrated that they were lacking the chemical dopamine. As a result, dopamine replacement therapy is now the mainstay of treatment of Parkinson’s disease. Secondly, the brains of people with Alzheimer’s disease have deposits (‘plaques’) made up of a protein called beta amyloid. Recent breakthroughs in the treatment of Alzheimer’s disease use antibodies, such as the drug donanemab, to clear ‘beta amyloid’ from the brain
Neuropathologists spend most of their time studying human brains. In contrast, many scientists study “models” of MND which can take two forms: either a non-human animal or cells kept alive in an incubator.
The animal models used are usually mice, fish or flies into which a MND-causing faulty gene has been inserted. While these animals have many factors in common with humans, they are also very different. For example, one of the key features of human MND is the degeneration of a long bundle of nerve fibres in the spinal cord called the lateral corticospinal tract. This is “lateral sclerosis” and is so important that MND is often called ALS “amyotrophic lateral sclerosis”. Mice, flies and fish do not have this tract.
Cell models involve growing cells in an incubator. Sometimes these cells come from people with MND, sometimes they have faulty genes artificially inserted into them. These cells that have grown for a few days or weeks have very little in common with the real motor neurons of a human. “Real” motor neurons have lived for decades, surrounded by other “support” cell types, are nourished by a constant blood supply, and have had the real experiences of human life: walking, eating, sleeping, exercising, and occasionally getting bashed around on a rugby pitch! While we still don’t know if there is a link between sport and MND, neuropathology is helping to research many different lifestyle factors that could lead to MND, including playing rugby and head injuries.

RELATED TOPIC
Blog | Charlotte Roy | 04 October 2022
While there are many similarities between model systems and real human nervous systems, these differences mean that any discoveries made in model systems need to be confirmed in real human neuropathology tissue to test their relevance. Finally, while a small number of people have MND because they have inherited a change in a single gene (“familial” MND), most have “sporadic” disease where no single identifiable gene is responsible. Neuropathology can generate data on both sporadic and familial disease, while most model systems only focus on familial forms alone.
What can we learn from neuropathology?
How has neuropathology helped move MND research forward?
Neuropathology can direct other scientists to look at particular areas of biology. For example, the most common motor neuron disease is called MND-TDP. It gets this name because there are abnormal deposits in the motor system of a protein called TDP-43. TDP-43 is strongly involved in RNA processing. RNA is a sort of “intermediary” copy of a gene used to make proteins.
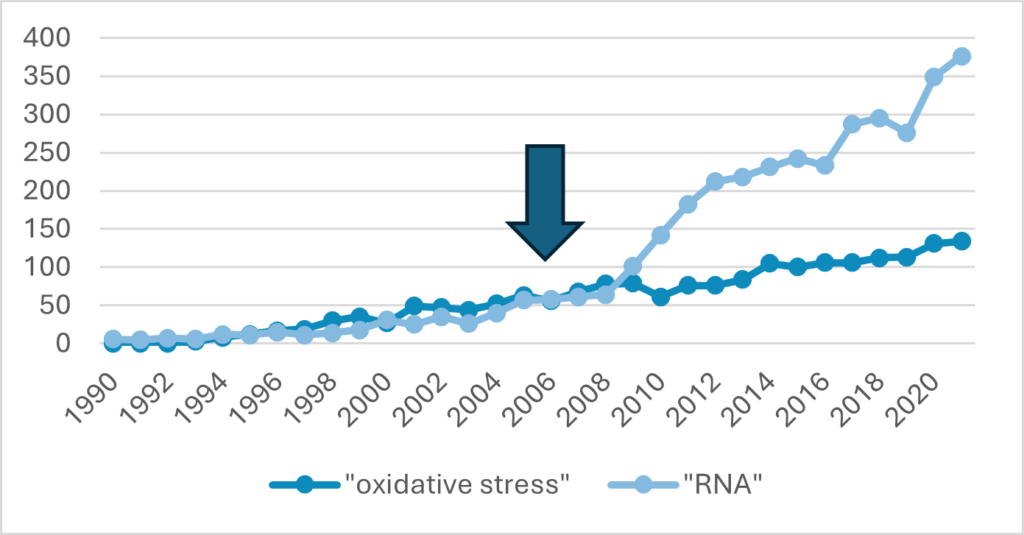
Scientists knew there was a protein deposited in MND for many years, but they did not know what it was until 2006 when neuropathologists showed it to be TDP-43. This caused a major shift in the attention of MND researchers and the number of scientific papers on RNA processing in MND surged. Before this discovery, the main area of research in MND was “oxidative stress”. You can see on the graph that published research on “oxidative stress” stayed around the same level whereas the number of scientific papers published on the subject of “RNA” in MND increased after the discovery of TDP-43.
The communication between neuropathology and other scientists is two-way: In addition to highlighting specific processes for model-based scientists to research, findings from model systems can be validated, and often extended in neuropathological studies. For example, a project I was recently involved in looked at components of the synapse (the machinery used for neurons to communicate with each other) in people who had a form of MND caused by inheriting mutations of a gene called C9orf72. A loss of key synapse components was found in mouse and cell models. Neuropathological studies confirmed this to be true of human MND as well. Importantly, neuropathology was able to add more detail to the finding: The loss was present in regions where the C9orf72 gene was most active, and in regions that received signals from cells that were most affected by TDP-43 pathology.
Neuropathology has also learned a lot of lessons from other neurodegenerative diseases that can be applied to MND. For example, all neurodegenerative diseases tend to start in one vulnerable part of the brain and then “spread” through the brain in a systematic manner. This “initiation and spread” was first described in Alzheimer disease, but has also been shown in most other neurodegenerative diseases, including MND. Any treatment for MND is likely to require focus on both initiation and spread to succeed. This is a bit like the way a wildfire may start in one vulnerable place (such as a place where people have barbecues) and then spread with the wind. If you want to reduce wildfire damage, it is important to both stop use of barbecues to stop initiation as well as putting in “fire breaks” to limit spread.
What are the factors that limit this work at the moment?
What are brain banks and why are they important?
Brain banks “do what they say on the tin”. People very kindly agree to donate their brains and spinal cords to brain banks after their death. When they die, neuropathologists harvest the brain and spinal cord and characterise the extent and nature of the disease processes present. The tissue is then carefully stored. The brain bank holds tissue from individuals with different kinds of motor neuron disease as well as people who did not have a neurological disease. This is highly skilled and labour-intensive work, and brain banks bring together the relevant scientists, doctors and mortuary staff who are capable of doing it.
When a scientist needs some brain tissue for a study, they can apply to a brain bank for this. The brain bank neuropathologists who have a lot of experience with this kind of research can advise what samples to use and how best to go about answering the scientific question.
Neuropathology plays a huge role in the science leading up to the discovery and development of new treatments for MND. Without tissue from people with the disease from brain banks, findings from models in the lab can’t be confirmed and can’t be used as targets for therapies. It is an essential part of the development and testing of new treatments for many diseases, including MND.
The importance of brain banks is reflected by the fact that there are UK-funded brain banks for the majority of neurological diseases. Unfortunately, most MND brain banks don’t receive the same funding as others and are a “side-project” for the Institutions that host them, and are supported by the Universities and NHS Trusts.
How could MND brain banks in the UK be improved?
At present, most MND neuropathology is done on a shoestring. This really clips the wings of neuropathology, but UK MND neuropathology would love to fly: In an ideal world, UK MND neuropathology centres would form a network (similar to the Brains for Dementia Research consortium). We would take MND and neurologically healthy control cases from almost anywhere in the UK at any time. Each case would have a very detailed characterisation using a “multi-omic” approach: This is where multiple aspects of the brain are assessed in multiple different ways including the genetic code, the amount of activity of different genes, the amount and location of proteins and the microscopic features of different parts of the brain. We would then co-ordinate this data with other large-scale data obtained from people with MND in life, such as the data from the MND register and co-ordinate this through the UK MND Research Institute. This would create a unique very large, very rich dataset that we would make available to MND researchers around the world.
How can people help neuropathologists to research MND?
You can find out more about tissue donation and contact details for brain banks in the MND Association’s information sheet. Please don’t contact the brain banks before reading the information sheet and checking that you are within the area that the brain bank covers.
We would like to thank Robin for giving his time to talk to us about his work and the role of neuropathology in MND research.
