On 29th September 2022 AMX0035, a treatment for Motor Neurone Disease (MND) was approved by the Food and Drug Administration (FDA) in the United States. Two countries have approved AMX0035, with Canada conditionally approving the drug, known there as Albrioza, back in June 2022. The Canadian approval is dependent on the results of the ongoing Phase 3 clinical trial, called PHOENIX. The FDA approval in the US is a welcome step forward in the fight against MND and further highlights the commitment and dedication of the research community in finding effective treatments. Approvals such as these would not be possible without the generosity and altruism of people living with MND, their families and carers. The community will now await the decision from the European Medicines Agency in early 2023 to see if the treatment could be approved in the UK and Europe.
In this blog we take you through the journey to the FDA decision for AMX0035, answering some frequently asked questions, as well as explaining what this approval means to people living with MND in the UK.
What is AMX0035?
AMX0035 is a combination of two drugs are already licensed to treat other conditions. These are sodium phenylbutyrate (PB) and taurusodiol (TURSO or TUDCA). Amylyx, the developers of AMX0035, have combined these two compounds to make AMX0035 to see if together they will slow the progress of MND, as measured by ALSFRS-R.
What does the drug do?
The two drugs that make up AMX0035 target the disease in slightly different ways. PB reduces the stress on the endoplasmic reticulum (ER), whilst TURSO blocks key cell death pathways. This dual approach is believed to improve the survival time of neurones.
Has AMX0035 been tested in a clinical trial?
AMX0035 has been tested in a Phase 2 trial (CENTAUR) with an open-label extension phase (OLE), in which all participants were given the drug. A Phase 3 trial (PHOENIX) began in October 2021, and is recruiting people with MND in the U.S., UK and Europe.
How was the CENTAUR Phase 2 trial designed?
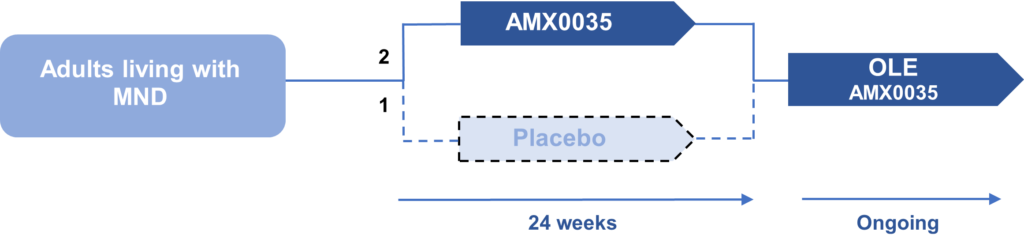
The trial was designed to be a randomised, placebo controlled, double blind trial for 24-weeks – meaning that the participants were either randomised into the treatment group (taking the drug) or the placebo group (dummy drug) for 24-weeks and neither the investigators or participants know which people are in each group (double blind). The primary outcome of the trial was physical function as measured by the rate of decline of the total score on the functional rating scale (ALSFRS-R) over the 24-weeks.
Who took part in the CENTAUR Phase 2 trial?
Participants were enrolled in the trial if they had an onset of symptoms within the previous 18 months. They were randomly assigned in a 2:1 ratio of AMX0035 to placebo. In total 137 participants were randomly assigned to the treatment drug (89 participants) or placebo (48 participants). Participants who completed CENTAUR were eligible for the open label extension phase of the trial after the 24 weeks, where everyone in the trial is offered the medication, even if they were originally put in the placebo group. Of the original 137 participants who were randomised, 90 entered the OLE.
What were the results of the CENTAUR Phase 2 trial?
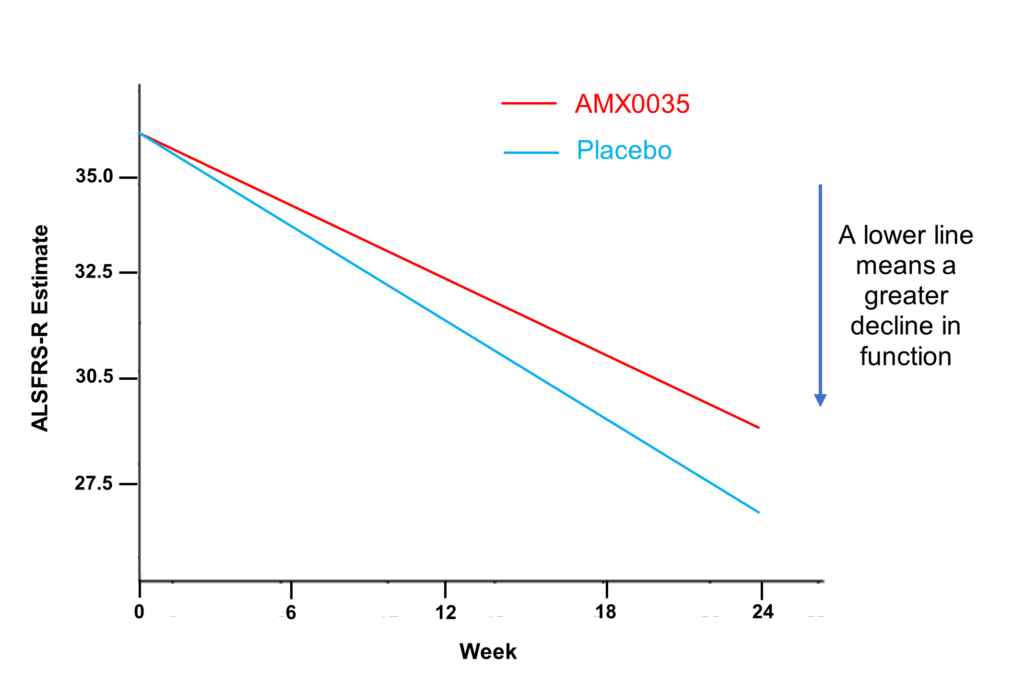
The primary outcome of the trial was the rate of decline of the ALSFRS-R score over the 24-week period. MND symptoms progressed in both groups indicated by the fall in ALSFRS-R in both groups. The average fall in the ALSFRS-R score was -1.24 points per month for the treatment (red line) and -1.66 points per month with placebo (blue line). This equated to a difference of 2.32 points at the end of the 24-weeks study which represents a relatively small slowing of disease symptoms.
What impact did AMX0025 have on survival?
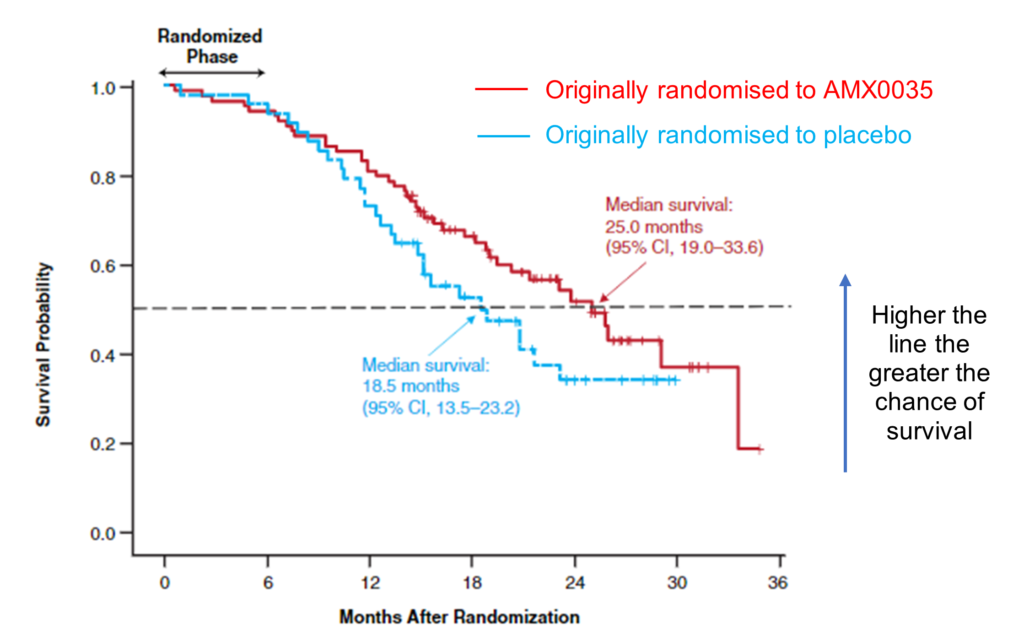
The median survival duration (that is the time until half of participants taking part in each arm of the trial either died or were put on permanent assisted ventilation or tracheostomy) was 25.0 months in the group being given the active treatment (AMX0035; red line) and 18.5 months in the group receiving the placebo (blue line). This means there was a 6.5-month difference in survival for those who received AMX0035 compared to placebo. Whilst this is a welcome step forward, this highlights that AMX0035 is not a cure but could increase survival for people living with MND.
Further analysis (using computer modelling) of the data after the trial ended to compare the people on the trial who received the treatment to historical data of people living with MND (a large database of information from people living with MND from 1992-2010 in Europe) found that there is potential for an 11-month increase in survival.
Were there any side effects of AMX0035?
Around 30% of participants who took AMX0035 reported to have gastrointestinal (GI) events within the first 3 weeks of the starting the treatment. After this initial 3 weeks on the treatment, the reporting of these events declined. The majority of the GI events reported were mild to moderate and could be overcome by reducing the dose temporarily and then increasing back to the original dose.
How can I access the drug?
Currently, the only way you can access AMX0035 in the UK is through a clinical trial. The Phase 3 clinical trial, called PHOENIX, is recruiting in the UK at:
- Plymouth – please contact the MND care coordinator on tracy.thomas9@nhs.net.
- Sheffield – please contact the Lead Research Nurse for MND on lee.tuddenham@nhs.net.
Additional sites are expected to open in the UK soon. For more information and to keep updated on new sites as they open, please head to the AMX0035 page on our website.
What does approval look like in the UK?
Amylyx have submitted a Market Authorisation Application (MAA) to the European Medical Agency for AMX0035. This application is based off the Phase 2 CENTAUR data and results. The EMA may decide that they need to see the data from the ongoing Phase 3 PHEONIX trial. The EMA decision is expected to be made in early 2023.
As the UK is no longer in the EU it is as yet undecided whether the UK will continue to be involved in EMA approval beyond 2022 or whether there will be a new approval process for the UK. We are in contact with Amylyx to see what approval will look like in the UK post 2022.
RELATED TOPIC
Blog | 19 January 2021 | Mandy Spencer
Virtual Symposium: Update on AMX0035 CENTAUR and open-label extension trials
AMX0035 is just one of the several potential treatments in clinical trials at the moment. The FDA approval, based on Phase 2 data, provides hope for a more rapid path to approval for other treatments under investigation in trials in the UK and across the world. This is especially true in the UK, with more clinical trials taking place than ever before, testing new potential treatments for MND. None of this progress is possible without the continued support of the MND community, the dedication and commitment of researchers and the generosity and altruism of people living with MND, their families and carers.
If you still have questions regarding AMX0035 and the PHOENIX trial, please see our FAQs or get in touch with the research team on research@mndassociation.org.
You can find additional information about AMX0035 in a statement by TRICALS here. TRICALS are a European research initiative uniting patients, researchers and ALS/MND foundations to achieve the goal of finding effective treatments for ALS/MND.

