A recent paper (October 2022), published in the journal Journal of Pathology: Clinical Research suggests that evidence of MND can be seen inside people years before they develop physical symptoms.
The paper titled ‘pTDP-43 aggregates accumulate in non-central nervous system tissues prior to symptom onset in amyotrophic lateral sclerosis: a case series linking archival surgical biopsies with clinical phenotypic data’ was written by Samuel Pattle and Judi O’Shaughnessy from Lothian Department of Pathology, Edinburgh, UK, and colleagues from the University of Edinburgh and University of Aberdeen, NHS Grampian and NHS Grampian Biorepository, Aberdeen.
TDP signature as a diagnostic for MND
The researchers looked for a particular ‘marker’ protein (called phosphorylated TDP-43) in samples that had been taken from people during routine hospital procedures, well before they developed any physical signs of MND.
Background Box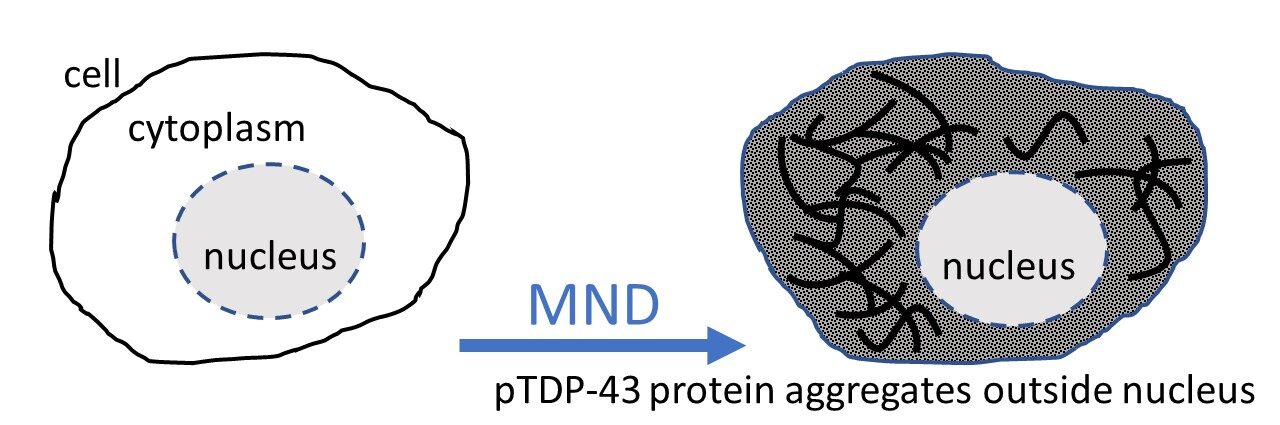
It has been known for a long time that in nearly all cases of MND, sticky aggregates or clumps of the protein TDP-43 can be seen in cells of the central nervous system (CNS) (such as in brain and spinal cord) in people who have had MND. These TDP-43 aggregates have been found in around 97% of all MND cases (with the exception of MND caused by a genetic change in SOD1 (around 2-3% of cases). In cases of MND, the protein is found outside the nucleus of the affected cells rather than inside the cell’s nucleus where the protein normally occurs. Seeing this mislocalised TDP protein in cells is considered a biological marker or signal of MND.
In theory, if it was possible to see inside living people and look to see if this protein signature is present in cells of their nervous system, it could be used as a tool to both diagnose MND and monitor progression of the disease over time. However, to remove pieces of the nervous system from people while they are alive to see if TDP-43 aggregates are present is not an option, because it would cause serious nerve damage. In contrast, small samples from other parts of the body are sampled or removed routinely in the health system, for example when biopsies are taken for cancers screening or an appendix or gall bladder is removed. Often samples of this tissue are taken (with permission) and saved for diagnostic and research purposes in a biobank/biorepository.
Design of the study
Previously the researchers had examined brain samples of 48 people who died with MND who had generously donated their brains to research biobanks in order to help further researchers understanding of the biology of MND. Every one of these 48 people had the signature TDP protein present in cells of their brains.
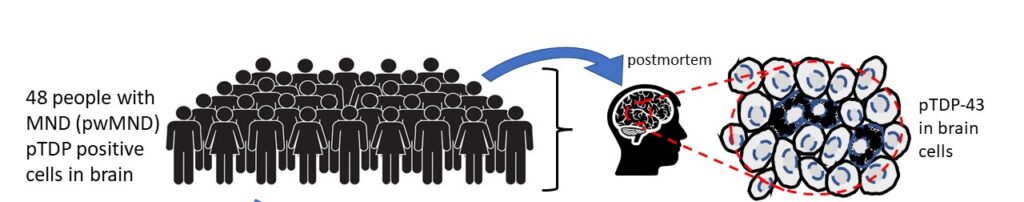
Following on from the previous research, this new study looked to see if any of the 48 people had any non-CNS tissue samples available in heath service biobanks. Of the 48 people they found that 13 people did have various samples of non-CNS tissue in the health service biorepository. In fact, a total of 68 different samples were actually available because some patients had several samples taken during their lifetimes, which were taken from different parts of their bodies (eg one person had samples of colon, lymph node, gall bladder, skin removed and stored at some point in their lives).
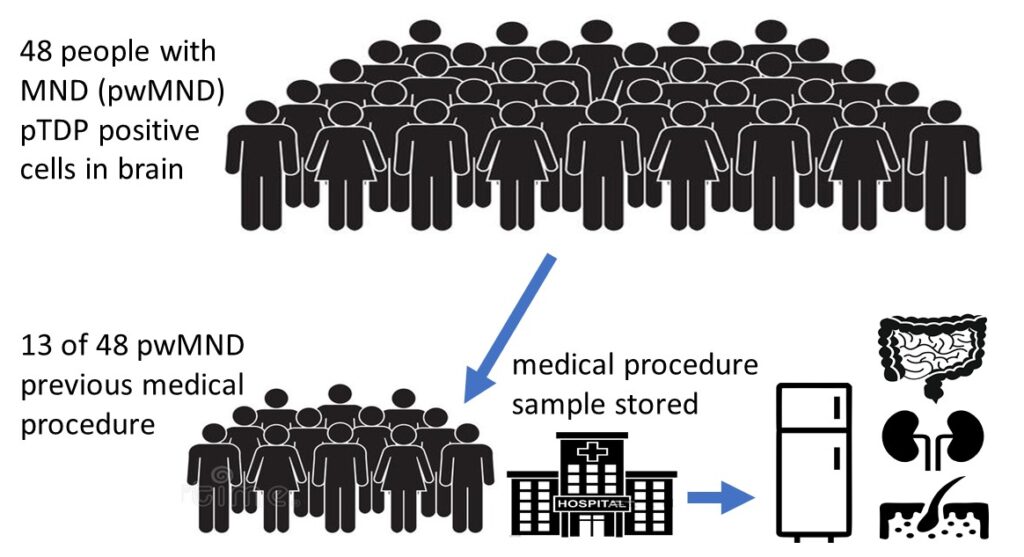
Background Box
In research studies it is important to use controls, as this allows researchers to confirm the results they are observing, and make sure the results are not due to the scientific method used or natural biology. The controls used in this study were non-CNS cells from people who never had MND. In the control group, the 3 people who never had MND, the researchers analysed their GI cells and found that in all three samples pTDP-43 aggregation and misexpression was not found.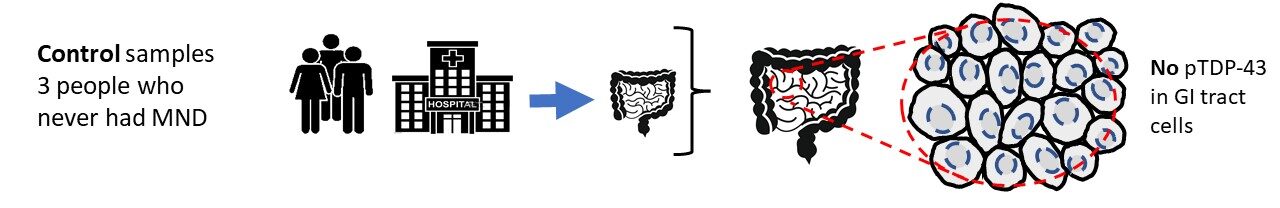
What did the study show?
The research showed positive pTDP-43-stained cells indicating mislocalised pTDP-43 aggregates present in cells from non-CNS tissue. This basically means that TDP-43 was found in other cells outside of the central nervous system. It is important to recognise that not all samples had positive cells and that only a relatively small number of samples were analysed.
Specifically, of the 68 samples looked at, pTDP-43 aggregates were identified in gastrointestinal (GI) tissue (two of two cases), lymph nodes (one of three cases), skin (two of eight cases) and blood vessel endothelial cells, which are a single layer of cells that lines the inside of blood vessels (6 of 22 specimens). The remaining samples showed no evidence of pTDP-43.
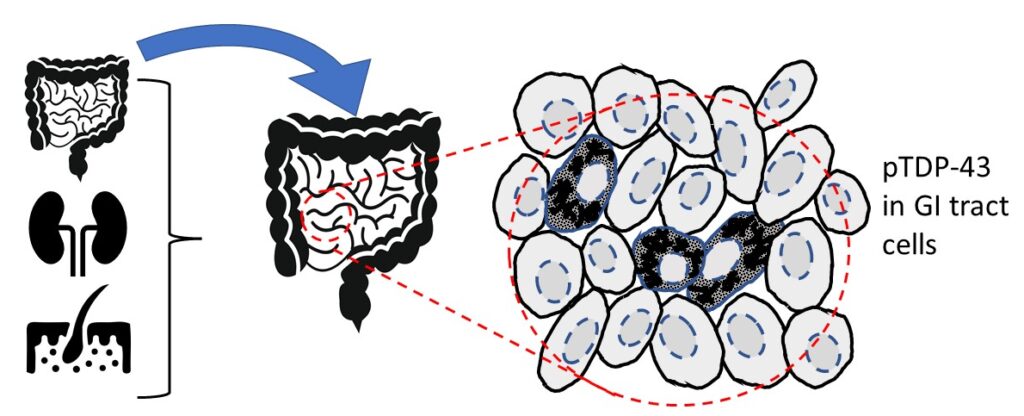
Both of the GI specimens evaluated were taken 2 months and 2 years prior to the persons MND diagnosis, and the lymph node sample that had pTDP-43 aggregates present was taken 14 years prior to the persons MND diagnosis. From this it is suggested that patients might have detectable signs of MND in cells that could be seen several years before physical MND symptoms. This suggests, at this time that the pTDP-43 found tissues outside of the central nervous system in the people who developed MND, could be a result of MND. However, further research is needed to accurately make this conclusion.
What does this all mean?
The results from this study could have quite a few potential implications. Firstly, it could help in the diagnosis of MND, specifically in the development of a method for earlier, easier and faster diagnosis, which is desperately needed. This could have a knock-on effect by enabling people to receive potential treatments far earlier than is currently possible, since they could be diagnosed earlier. We know that the earlier a treatment is given, the greater the chance it has of having a beneficial impact.
Additionally, this research could help in our understanding of MND. For example, highlighting possible new sites of onset within the body. Understanding the disease and everything that goes wrong within the body is key to finding effective treatments and the fight against MND.
Whilst, this research could have potential important implications, it is important to note that more research is still needed in this area before it could be used in the clinic. The authors themselves state that the study used a relatively small number of samples, as they only used samples from 13 people. They also only looked at 3 control samples. Larger additional studies, with a larger number of control samples, are required to confirm the results found in this study as it could be found that there are other reasons, other than MND, that lead to having TDP-43 aggregates in non-CNS tissue. We know that TDP-43 is present in every one of our cells and is needed for their function, but we don’t yet fully understand everything TDP does. This means that it is possible that some of the cells that were found to have pTDP-43 are due to natural cellular processes that are not yet fully understood.
If the findings of this study are confirmed in additional studies and pTDP-43 aggregation is present in other tissue throughout the body in only people who develop MND then there is a real potential of using this to develop a screening and/or early intervention tool long before neurological symptoms occur. Additional development would also be needed in the creation of the screening/early intervention tool as it would only be practical to use more accessible tissue types, such as skin or cheek cells. This is a really interesting study, and we look forward to hopefully reporting on additional larger studies that confirm these findings.
References
Rifai, O.M., Longden, J., O’Shaughnessy, J., Sewell, M.D., Pate, J., McDade, K., Daniels, M.J., Abrahams, S., Chandran, S., McColl, B.W., Sibley, C.R. and Gregory, J.M. (2022), Random forest modelling demonstrates microglial and protein misfolding features to be key phenotypic markers in C9orf72-ALS. J.Pathol.. https://doi.org/10.1002/path.6008
Gregory JM, McDade K, Bak TH, Pal S, Chandran S, Smith C, Abrahams S. Executive, language and fluency dysfunction are markers of localised TDP-43 cerebral pathology in non-demented ALS. J Neurol Neurosurg Psychiatry. 2020 Feb;91(2):149-157. doi: 10.1136/jnnp-2019-320807. Epub 2019 Sep 12. PMID: 31515300; PMCID: PMC6996101.
