Despite decades of research, we still do not fully understand why some people get MND, but studies in cell and animal models of the disease suggest that astrocytes and microglia cells are key players in the process, and a potential target for new therapies to moderate oxidative stress, reduce mitochondrial damage, and limit glutamate excitotoxicity – all thought to be causes of MND.
In recent years, plant-derived compounds have been studied in neurodegenerative diseases for their neuroprotective qualities and glial cell response. A review by Oliveira and colleagues (2023) – Impact of Plant-Derived Compounds on Amyotrophic Lateral Sclerosis – describes the mechanisms of action of natural compounds associated with neuroprotective effects, and the possibilities for new therapeutic strategies for MND.
It must be made clear that very few studies have been carried out in humans for the compounds that will be discussed in this blog article. In fact, for most, the only studies so far have been in animals. As such, these are not tried and tested treatments for MND. The information in this blog article should not be taken as dietary or medical advice. This is a summary of the paper published by the authors above, together with some supplemental information provided by the author of the blog. There may be other research that offers an alternative view.
What are astrocytes and microglia?
Astrocytes and microglia are both glial cells and play important roles in the central nervous system (CNS). Glial cells hold nerve cell, or neurons, in place and help them to work in the way they should.
Astrocytes
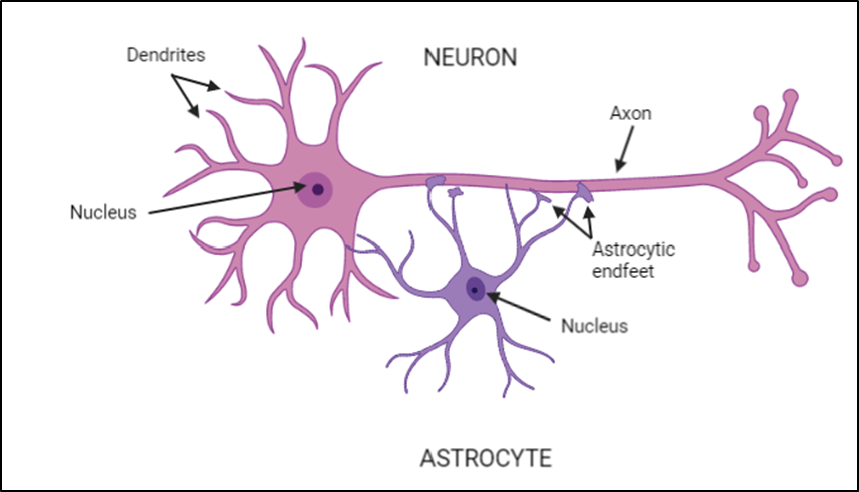
Astrocytes have a number of roles in the CNS. They are involved in the immune response; they secrete, absorb and regulate neurotransmitters (which help to move electrical impulses from one nerve cell to the next); they provide nutrients to nerve cells; they help to repair damage to the brain and spinal cord following infection or injury and they help to maintain the blood-brain barrier, which stops harmful substances from reaching the brain.
Microglia
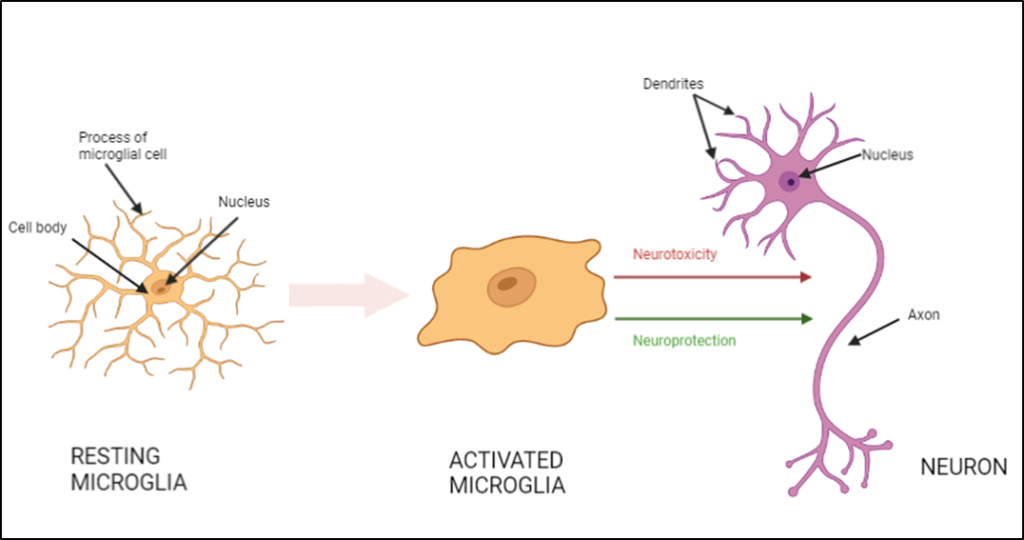
Microglia are constantly moving around the CNS identifying damaged nerve cells and infectious substances to help maintain the proper balance in the CNS. Microglia are able to change their structure in response to changes in the CNS and will react quickly to decrease inflammation and destroy infection-causing agents that have passed through the blood-brain barrier. This is known as the M2 state. However, the immune response can quickly become harmful as microglia can release chemicals into the space between cells such as hydrogen peroxide and glutamate which can damage cells and cause cell death, known as the M1 state.
The role of astrocytes and microglia in MND
One of the possible causes of MND is mitochondrial dysfunction. Mitochondria are small structures in cells that are found in the fluid that surrounds the nucleus – the cytoplasm. Mitochondria make most of the energy that the cell needs to perform its function. If mitochondria are damaged this can cause too many unstable molecules called free radicals in the body, and not enough antioxidants to remove them. This can trigger glutamate excitotoxicity, leading to the activation of astrocytes which disrupts glutamate uptake, consequently leading to further excitotoxicity in motor neurons.
Another feature often seen in people with MND (except those with a SOD1 mutation) is the toxic build-up of the protein TDP-43. This is found in the cytoplasm of motor neurons, and also in glial cells in all people with sporadic MND and inherited MND, except that caused by a SOD1 mutation.
The concentration of glutamate outside cells is tightly regulated by transporters of neurons and astrocytes. In MND, the levels of glutamate outside cells are increased causing glutamate excitotoxicity. Among other things, this could be caused by a decrease in glutamate re-uptake in the astrocytes surrounding neurons and impaired mitochondrial function. One of the most important glutamate transporters – EAAT2 – is expressed by astrocytes. The decrease in the expression of EAAT2 in people with MND suggests that failure of astrocytes to clear glutamate excess at the synapse (the space between the end of a neuron and another cell, across which nerve impulses are carried by neurotransmitters) contributes to the degeneration of motor neurons by excitotoxic mechanisms.
There are also several studies that suggest neuroinflammation plays a major role in the onset of MND. In MND, neuroinflammation is triggered by activation of microglia and the immune system and, in MND, activated microglia initiate a process which ends with the formation of a highly toxic compound, called peroxynitrite, which can combine with glutamate and trigger cell death. It has been seen in mouse models of MND that microglia change from their M2 neuroprotective state to the M1 neurotoxic state, as discussed earlier in the blog, as MND progresses.
Treating MND today
Until recently riluzole, which blocks the neurotransmitter glutamate, and edaravone which is an antioxidant, were the only drugs licensed to treat MND, with only riluzole available in the UK. In June 2022 and September 2022, AMX0035 was approved for the treatment of MND in Canada (marketed as Albrioza) and the USA (marketed as Relyvrio) respectively. In April 2023, Tofersen (marketed as Qalsody) was approved for the treatment of MND caused by a mutation in the SOD1 gene in the USA. None of these drugs are a cure.
Plant-derived bioactive compounds, which are a type of chemical found in plants and certain foods that may have actions on the body that promote good health, have been widely investigated due to their anti-inflammatory and antioxidant properties, as well as other effects associated with protein expression, waste removal, cell death and inhibiting the toxic build-up of proteins, which makes them potential compounds to develop into new treatments for MND.

RELATED POST
Blog | 3 October 2018 | Mandy Spencer
The effects of ashwagandha in a SOD1 mouse model of MND
How are potential new treatments studied?
In the early stages of drug discovery, cell models (models ‘in a dish’) of MND are used to understand what is happening inside motor neurons and to find compounds that may target these events. In recent years, glial cells have been used as models of MND – a notable development as these cells appear to have an important role in cell death and survival.
But, no matter how advanced cell models have become, they cannot be used to assess how a drug behaves in a whole organism. To understand how potential new treatments affect other cells, animal models of MND are needed. The first mutation-specific mouse model of MND was developed in 1984, when a mouse was produced with a SOD1 mutation and, since then, mutations in other animals have been successfully reproduced. However, even though SOD1 models are considered the ‘gold standard’ in MND studies, every model has its limitations and there is no model capable of fully replicating human MND. The following plant-derived compounds have been studied in animal models. Any future studies in people may not produce the same results.
Using natural compounds in models of MND
For thousands of years, plant-derived remedies have been used in traditional medicine throughout the world, and plant-derived compounds would seem to have a place in modern pharmacology and the treatment of neurodegenerative disease. These molecules, or secondary metabolites, are not related to plant growth, but rather secondary functions related to how the plant adapts to ‘biotic’ and ‘abiotic’ stress.
Biotic and abiotic factors are what make up an ecosystem. Biotic factors are living things within an ecosystem such as plants, animals and bacteria. Abiotic factors are non-living components such as water, soil and atmosphere.
Plant-derived compounds seem to act in four interconnected mechanisms in animal models of MND:
- As an antioxidant because of their ability to harvest free radicals (the cause of oxidative stress in cells)
- As anti-inflammatory agents
- As biochemical chaperones, that moderate proteins and prevent toxic clumping
- In molecular signalling, interacting with molecules that promote cell survival and changes to stress.
Flavonoids

Flavonoids are secondary metabolites found in vegetables, fruits and some drinks such as tea and wine and are said to promote a wide range of health promoting benefits. Flavonoids are split into six sub-classes, each with its own structure, which allow it to act as an antioxidant, anti-inflammatory and anticarcinogenic agent because these variants are able to modulate gene expression – the process by which instructions in our DNA are converted into a functional product, such as protein – and related enzymes and pathways.
In the past few years, studies have pointed to flavonoids as important biomolecules in potential new therapies for neurodegenerative diseases. They offer protection against oxidative stress, nerve cell death caused by the toxic build-up of proteins, the over-production of glutamate and microglial activation.
Although there have only been a few studies using animal models, so there is no evidence of effectiveness in people with MND, flavonoid use has produced some promising results. The antioxidant properties of a particular flavonoid derived from drinks like green and black tea increased lifespan, preserved nerve cells, reduced microglial activation and decreased oxidative stress. Compounds from other sub-classes of flavonoids have been found to inhibit the toxic accumulation of SOD1 protein, and it was shown that this was not related to the antioxidant properties of flavonoids as the antioxidant control failed. Again, this has been seen in animal models of MND only, and the flavonoid compounds used were given in concentrated formulations, far higher than would be found in the consumption of foods and drinks containing flavonoids. This is true for all of the compounds discussed in this blog.
These multiple molecular mechanisms seem to indicate that flavonoids offer neuroprotection in animal models of MND and that the effect of the flavonoid can be linked to its structure, meaning different flavonoids can have different effects. More studies in animals are needed before testing can begin in people, especially to understand the effect of specific flavonoids and the correct dosage.
Stilbenes

The most commonly known stilbene compound is resveratrol, found in the diet in grapes, red wine and peanuts. Resveratrol is thought to act as an antioxidant.
Resveratrol has quite a simple chemical structure that allows it to interact with a number of receptors and other targets, and different pathways connected to cell survival like SIRT-1. SIRT-1 is involved in cell cycle regulation, DNA repair, programmed cell death (apoptosis) and inflammation.
Studies using cell models of MND have found that resveratrol reduced neurodegeneration and protected motor neurons from stress through SIRT-1 activation.
Studies in SOD1 mouse and rat models of MND had similar results concerning activation of SIRT-1 and reduction in MND severity. In the mouse model, resveratrol injections extended survival, possibly by inhibiting motor neuron loss. In the rat model, resveratrol given orally showed that treated rats had increased levels of SIRT-1 in their motor neurons, which delayed disease onset and mobility issues, increased motor neuron function, reduced spinal motor neuron degeneration and reduced microglial activation.
Other animal studies have also shown resveratrol to be activated by other mechanisms, leading to protection against glutamate excitotoxicity and the toxic build-up of the SOD1 protein.
ALS Untangled systematically reviews alternative and off label treatments to try and help people living with MND to make more informed decisions about them. They have carried out a review of resveratrol which concluded that the compound may confer benefits in animal models of SOD1 MND. At the point of publication (2019), no trials had been carried out in people with MND, but trials in other populations reported problems such as weight loss and kidney damage and therefore ALS Untangled did not recommend resveratrol as a treatment for MND at that time.
However, there is now a Phase 2 clinical trial underway in Spain that is looking at the combined effects of curcumin and resveratrol with the drug G04CB02 (currently marketed for the treatment of several conditions), which is thought to act in a similar way to riluzole and/or edaravone in MND. The estimated completion date (that is, the date the researchers think the last participant will receive the final dose) is June 2023. It will be several months before any results are published.

RELATED POST
Blog | 23 October 2019 | Mandy Spencer
ALS Untangled – untangling the mysteries of alternative and off-label treatments
Curcuminoids

Curcumin is an orange-yellow powder, commonly known as turmeric. The herb has long been used in traditional medicine for a diverse range of conditions. Commercially available curcumin is a mixture of three curcuminoids: curcumin; demethoxycurcumin (DMC); and bisdemethoxycurcumin (BDMC).
Curcuminoids have been extensively studied for their anti-inflammatory, antimutagenic and antioxidant effects, and some of these studies have shown that curcumin could also be important in the prevention of neurodegeneration through the regulation of gene expression and mitochondrial protection.
In models of MND a derivative of curcumin, known as Compound C, successfully protected motor neurons from toxic build-up of TDP-43, which can lead to cell death, and reduced oxidative stress. DMC has been shown to increase mitochondrial stability. In a clinical trial, curcumin was associated with better ALSFRS-R scores and with improved cellular energy production.
In 2018 ALS Untangled carried out a review of the evidence for curcumin as a potential therapy for MND. Based on their findings, Dr Richard Bedlack (founder of ALS Untangled) led a small clinical trial of a water-soluble form of curcumin called Theracurmin in 50 people with MND, who took it for six months. This showed no effect on disease progression.
Phenolic acids

Phenolic acids are easily absorbed through the digestive tract and are beneficial to human health due to their potential antioxidant properties and their ability to promote anti-inflammation. In the diet they can be found in wholegrains, cocoa, fruits, nuts, and coffee and beer. They contribute greatly to the taste, flavour and odour of plants.
In 2010, Shimojo and colleagues used an animal model of MND to test an extract of rosemary – rosmarin – and two of its main phenolic acids: rosmarinic acid (RA) and carnosic acid (CA). Animals treated with the extract and RA showed longer survival, increased motor function, didn’t lose weight as quickly and had reduced degeneration of some motor neurons. CA also had an effect on motor function, but RA appeared to be much more effective against the progression of MND in these animals. Another study from 2018 showed that both RA and CA shared neuroprotective qualities when examined in neurons in a dish. Further pre-clinical studies (in animals) should explore both the individual therapeutic effects of RA and CA and the potential complementary effects of these compounds on neurodegenerative disease progression.
Terpenes

In plants, terpenes are the major constituents of resins and essential oils. In the diet they can be found in citrus fruits, tea and thyme. They are also found in cannabis.
Terpenes have a wide range of uses and are found in pharmaceutical drugs, cosmetics, food and beverages, biofuel and rubber derivatives. They have also been described as having anticancer, antimicrobial, antifungal, antiviral, antihyperglycemic, analgesic, anti-inflammatory and antiparasitic properties.
There have been several studies that have demonstrated potential neuroprotective effects of terpenes such as a decrease in programmed cell death (apoptosis), reduction in products of oxidative stress and stabilisation of mitochondria. Derivatives of the terpene oleanolic acid, found in olive oil, have been found to increase antioxidant defence in mouse models.
Because of the broad spectrum of action of terpenes, they could be good candidates as treatments for neuroinflammation, oxidative stress and glutamate excitotoxicity but further studies in animal models are needed before any potential treatments can be trialled in people with MND.

RELATED POST
Blog | 24 January 2019 | Mandy Spencer
Cannabis-based products for medicinal use
Coumarins

Coumarins, found in cinnamon, tonka beans and sweet clover, are a large family of compounds from natural and synthetic origins and have been extensively studied for their antitumour, anti-inflammatory, antiviral, antibacterial and neuroprotective qualities, to name just a few.
Plant extracts containing coumarins have been studied in different models of neurodegeneration, including MND, and have been shown to have neuroprotective effects.
Carotenoids

Carotenoids are yellow, orange and red pigments found in a diverse range of plants and food such as pumpkins, grapefruits, tomatoes, bell peppers, leafy green vegetables, and broccoli. They are also found in egg yolk and are very easily absorbed and used by the body from this source.
In neurodegenerative disorders, carotenoids are potent antioxidant and anti-inflammatory agents, reducing oxidative damage in models of neurodegenerative disease. However, there are not many models that look specifically at their effect on MND.
A 2013 case-control study by Fitzgerald and colleagues composed of more than 1 million individuals with more than 1000 cases of MND, pointed to the consumption of beta-carotenes as protective agents against the risk of MND. However, no further studies have been carried out in people and these are needed to better understand the role of carotenoids, particularly beta-carotenes, in MND.
Going forward
Another recent study ‘Therapeutic implications of some natural products for neuroimmune diseases: a narrative of clinical studies review’ (Wijeweera and colleagues, 2023) also looks at the use of naturally derived compounds, including curcumin, catechins (found in fruits such as apples, cherries, apricots, strawberries and blackberries, and in black and green tea), gingko biloba, ashwagandha, ginseng, cannabis and more to treat diseases such as MND, Alzheimer’s disease, multiple sclerosis and others. They conclude that there is evidence to suggest that these natural products have therapeutic potential and further studies are needed to determine the correct techniques to convert natural products into probable drug candidates. They suggest that the development of such ‘nutraceuticals’ – which are foods containing health-giving properties – may pave the way toward new therapeutic strategies to help combat chronic neuroinflammation and overcome neuroimmune disorders.
To further study this area of potential therapeutics, the University of Westminster has opened a Centre for Nutraceuticals – a first-of-its-kind initiative in the area of nutraceuticals, supplements and functional foods, looking at how the power of these natural compounds might be harnessed to fight disease.
Although plant-derived remedies have been used for thousands of years in traditional medicine, this is still a relatively new area of research for tackling neurodegenerative diseases like MND, and we are still a long way from turning any of these compounds into new treatments. The compounds used in the animal models mentioned are concentrated forms and equivalent amounts, and therefore any potential benefits stated in studies of animal models, would not be obtained from eating the foods listed as part of a healthy diet.
The information in this blog should not be taken as dietary or medical advice. Consult your GP or neurologist before undertaking any changes to your diet, or before beginning any supplementation.
