In June we hosted the second MND EnCouRage UK event for early career researchers (ECR’s) which aims to support them to continue working in the field of MND. The event included lots of talks and workshops from senior researchers to provide tips and advice on moving forward in their careers and help them to develop new skills in areas like presenting their work to non-scientific audiences. We also challenged the ECR’s to write a blog to explain their research to the MND community. This guest blog is from Marianne King, one of the ECR’s who came to the event this year.

My name is Marianne King and I am a postdoctoral researcher at the Sheffield Institute for Translational Neuroscience (SITraN).
I had always enjoyed science, particularly human biology, and wanted one day to help “cure diseases”. When I was nine years old my grandmother was diagnosed with Alzheimer’s Disease, and I experienced how heart-breaking neurodegenerative diseases can be. I naively promised her that one day I would cure Alzheimer’s Disease, thinking at nine that this might be an achievable possibility for one person. She died when I was fifteen, just in time for when I had to start making serious decisions about my future. I decided I’d like to become a researcher.
I ended up studying Biomedical Science at the University of Sheffield so that I could learn more about health and disease. During this degree I learnt about MND for the first time and something about it affected me, as well as the fact I found it fascinating. I sent a skyward apology to my grandmother, telling her that I’d like to work on MND instead, and that I hoped she wouldn’t mind. I started a master’s degree at SITraN, also at Sheffield, where I was able to work on an MND research project. When this finished, I applied for PhDs so that I could start my career in research.
My PhD wasn’t quite on MND (it was on a neurodevelopmental disorder called Rett Syndrome), but I really enjoyed it, and I was determined to return to MND research. When a postdoctoral position opened up at SITraN looking at the different types of cells in MND I applied immediately, and I was lucky enough to be hired for my first postdoc.
My current work focuses on looking at the cell types that are affected in MND and how they impact each other. Motor neurons, the main cell type affected in MND, connect our brains and muscles. This connection is what allows us to move. In MND, these cells start to die, which is what leads to progressive paralysis. But motor neurons aren’t the only cell types affected by MND. They are surrounded by many more cells called glia, which have roles in keeping our motor neurons healthy.
Glia cells include star-shaped cells called astrocytes. These cells are like motor neurons’ best friends, clearing up waste the neuron produces, supplying them with energy when they need it, and helping them form vital connections with each other.
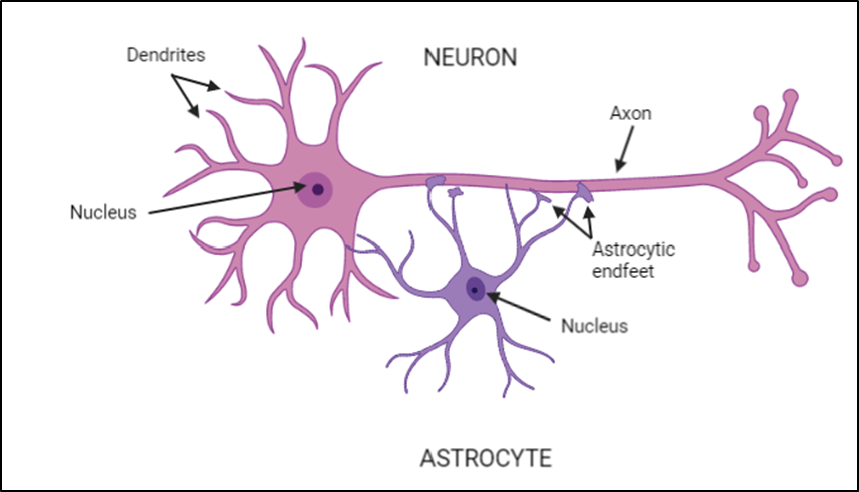
Another type of glial cell are called microglia, the brain’s resident immune cells. They help deal with infection, clearing up any dead cells, and helping the neurons form connections.
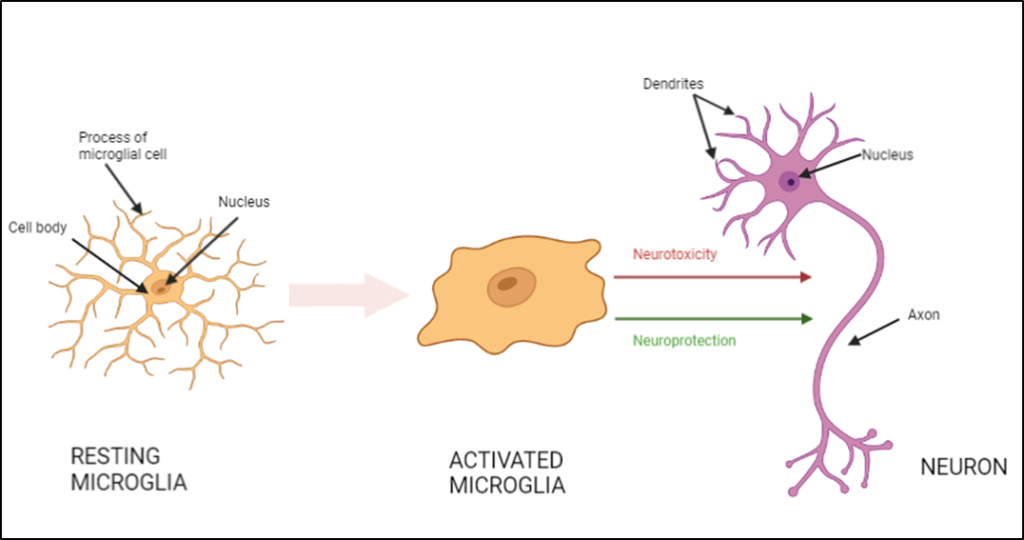
Astrocytes can also communicate with microglia, and vice versa. It’s a bit like these cells, alongside the motor neurons, are in a constant 3-way telephone call with each other.
In healthy conditions, this telephone call and communication is harmonious, and everyone gets along well. In MND, the microglia and astrocytes get angry, which we call “reactive”. Instead of supporting the motor neurons and each other, they can become actively toxic and stop providing energy. The 3-way telephone call is no longer the supportive environment it once was. This puts great stress on the motor neurons, and it contributes to their death.
My work is trying to find out more of what is happening in this reactive and angry conversation. Who becomes angry first, and what triggers that? What toxic things are the astrocytes and microglia releasing that kill the motor neurons? Is there anything they stop releasing? Is there any way we can intervene?
To do this, we have to grow motor neurons, astrocytes, and microglia together. Usually in the lab these cells would be grown on a flat surface, in what we call 2D cell culture. Whilst being hugely useful cultures, our brains are not 2D. They’re hugely complicated, wrinkly 3D organs. This is why, in my project, we are trying to grow these cells together in a 3D way. It is hoped that this will mean they grow in a way that is more similar to how they might grow in our actual brains.
It isn’t possible to take these cells directly from people. Instead, we take skin biopsies from healthy people and from people living with MND. Using a combination of different chemicals, it is possible to take these skin cells back to a stem cell state. From stem cells they can be turned into any cell type we want in the lab, including motor neurons, astrocytes, and microglia. The benefit of using these stem cells is that the brain cells we make from them will have all the information from the original person, including any MND-causing genetics. This makes them a very powerful tool for looking at any differences in brain cell function between healthy individuals and those living with MND.

How is it possible to grow all these cells in a 3D way? As I mentioned before, we would usually grow our cells on a flat surface, on the bottom of a plastic dish. The bottom of the dish is coated in a gel rich in chemicals that the cells love; they attach to it and grow very happily in a flat sheet.
To grow cells in 3D, we instead embed the cells inside this gel rather than on top of it. This gel-cell mixture is then added to special dishes that allow the cells to grow in a cylinder shape, in a proper 3D structure.
It is possible to let the cells grow together in this gel, and they grow and interact in a way that is quite different to how they’d grow in 2D. Reaching the point where all the cells are made, and then making sure that they survive in the 3D structure, and that it is possible to image them (so we can see what’s happening), has taken me a long time, but I am very excited to see what we can discover using this system.
I hope that because these 3D structures mimic our brains more closely than 2D ones, that anything we find out will be more likely to translate better to the clinic. We are also hoping to test gene therapies and drugs in these cultures, and again it is hoped that the results from these will be more applicable for people with MND. I see my work as a useful tool to study MND with, and I hope, even if it’s in a small way, that it will help people who live with MND.
We would like to thank Marianne for taking the time to write this guest blog about her work and also thank everyone involved in making MND EnCouRage UK 2023 such a success.
Thank you very much Mariann!