 Head injury has been a hot topic in the media in relation to MND. I also receive a number of enquiries from people living with MND asking about the causes of MND, and whether past head injury may influence this? This very topic was discussed in the epidemiology session on the second day of the 25th International Symposium on ALS/MND.
Head injury has been a hot topic in the media in relation to MND. I also receive a number of enquiries from people living with MND asking about the causes of MND, and whether past head injury may influence this? This very topic was discussed in the epidemiology session on the second day of the 25th International Symposium on ALS/MND.
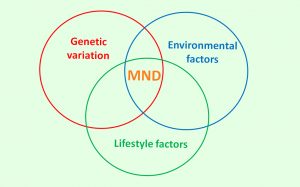
We know that the majority of cases of MND are caused by a combination of subtle genetics, lifestyle and environmental factors. We have identified some of the genetic factors involved; however the environmental and lifestyle factors remain somewhat elusive.
Head injury
To date, there has been mixed results on head injury and the risk of MND. Dr Christina Fournier said: “We wondered whether head injury could trigger the disease, cause faster progression and an earlier age of onset.”
Dr Fournier recruited 100 people who had been diagnosed with ALS (the most common form of MND) from a clinic in America. 24 of these had head injury, whereas 76 did not.
She looked at all the factors such as the ALS Functional Rating Scale (ALSFRS) and found that head injury did not affect age of onset or the progression of the disease in these individuals. Therefore, she concluded that there was no association with head injury and the rate of ALS.

Looking further into the brain
Dr Fournier, however, wanted to look further and find out whether there were any pathological findings relating to head injury and ALS. She did this by looking at 47 autopsy cases, of which 9 had experience of head injury.
We know that the protein TDP-43 is found in clumps within the motor neurones and brains of people with MND. Dr Fournier wanted to find out whether this protein was found in increased amounts in those who had head injury, to find out if this triggered the disease process.
Dr Fournier said: “We found that there was no difference in the pathological findings in the brain compared to ALS cases with no head injury history. Therefore, this study does not suggest that head injury plays a role in inciting the degenerative pathways involved in ALS.”

Diabetes and MND?
Dr Daniela Mariosa also presented her research during the epidemiology session. She presented some really interesting results on diabetes and MND.
Using a Swedish patient population-based register from 1987 she investigated whether diabetes was a risk factor for MND by studying 224 cases and 1,437 controls.
Dr Mariosa said: “Our research in Sweden has shown that people who were diagnosed with diabetes before the age of 30 were at an increased risk of MND.
“However, interestingly, if people were diagnosed with diabetes after the age of 30 then they were at a decreased risk of developing MND. This makes diabetes a risk factor if diagnosed before the age of 30 but a protective factor if diagnosed after this age.”
It was reassuring to know that a questioner from the audience also found similar results in their study, confirming further research is needed to investigate diabetes (including the different types) in relation to MND.
Military service
Another talk that caught my attention was one by Dr Marc Weisskopf on military service and ALS, another hot enquiry topic!
D Weisskopf found that the overall risk of developing ALS in his study was 20% higher in those who undertook military service. He also mentioned that those who underwent military service were twice as likely to smoke.
This is important because smoking has been previously identified as a potential risk factor for MND. However, Dr Weisskopf said that this was found not to affect the results of this study.
Dr Weisskopf said: “Our results are the first to examine the question of the association between military service in general—that is not restricted to service in a specific conflict—and the risk of ALS since the first report of this almost 10 years ago. Unlike the prior report, our current one is in a population that is representative of the US non-institutionalized population.
“The results reinforce the finding of an increased risk of ALS among those who serve in the military, although our recent findings focus attention on those who served during World War II. Further study of military veterans is needed to identify specific risk factors associated with military service that could account for the increased risk.”
Because this research was on US military veterans, a questioner from the audience asked if there had been any non-US military studies? Interestingly there has only been one non-US study, which was conducted in France. Therefore it seems more research is needed on non-US studies in this area.
Final thoughts
Researchers are beginning to understand the causes of MND. From this year’s epidemiology session it can be seen that researchers are making real head way in identifying the elusive environmental factors involved in the disease, bringing us closer to our vision of a World free from MND.
After you’ve finished reading the symposium articles that interest you, we’d be grateful if you could spare a few minutes to fill in our short online survey on our symposium reporting. Your comments really are useful and will allow us to continually improve our symposium reporting https://www.surveymonkey.com/s/NBGZR5S
I am from UK. Diabetes is inherited in my family. My dad got it first when he was 30 yrs. I was then diagnosed when I was 7yrs in 1987, my sister was diagnosed at 3yrs in 1986, my mum was diagnosed in 1999 in her 50s. All type 1 diabetics. My mum was 6 yrs old when she got mnd in 2012 and died from it in 2013. She went downhill rapidly losing most of her capabilities within a few months and then lingering in her body if a prison for a year. She was a smoker but absolutely no military background