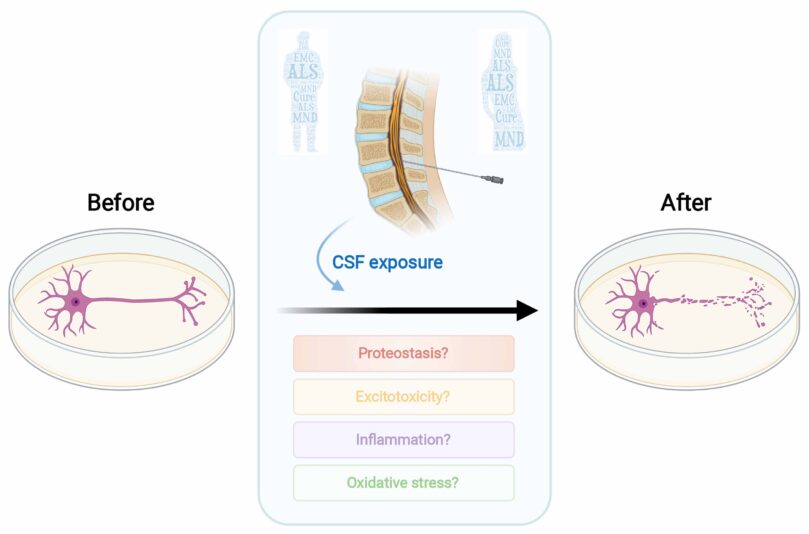
A new way to detect faulty TDP-43 in MND
Reading Time: 7 minutes Researchers from the University of Aberdeen and the University of Edinburgh have developed a new tool that could help to detect signs of MND in cells before symptoms of the disease start. This work was recently published and was previously presented at the 34th International Symposium in Basel by Dr Jenna Gregory. The new tool…