 Association-funded PhD student, Helena Chaytow (Royal Holloway, University of London), is using DNA to develop a targeted treatment for MND. Now entering her final year, we report on what she’s achieved so far and her future plans.
Association-funded PhD student, Helena Chaytow (Royal Holloway, University of London), is using DNA to develop a targeted treatment for MND. Now entering her final year, we report on what she’s achieved so far and her future plans.
The background
Helena’s research is looking at the chemical messenger ‘glutamate’. Glutamate is released by motor neurones in order to stimulate a nerve impulse from one motor neurone to the other, which is how the instruction to move our muscles travels from our brain to our limbs.
In order to pass the message on, glutamate needs to bind to the second nerve cell, and it does this by acting like a ‘lock and key’. Glutamate acts as a key, opening its specific lock (receptor) on the second nerve cell. This causes the nerve cell to open up and fill with several molecules including calcium, triggering the second nerve cell to pass on the nerve impulse (see image below).
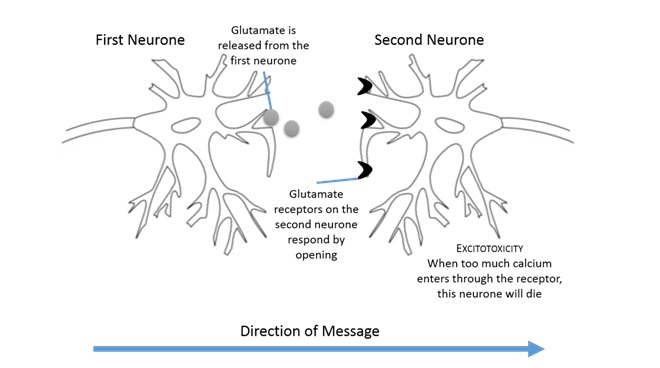 However, too much glutamate can be toxic to motor neurones causing ‘excitotoxicity’. Excitotoxicity is one of the mechanisms believed to cause motor neurones to die in MND. An overload of glutamate can cause the motor neurone to be constantly ‘open’, leading to an excess build up of calcium within the cell. This build up of calcium eventually causes the motor neurones to die. Stopping this glutamate overload is key to Helena’s research.
However, too much glutamate can be toxic to motor neurones causing ‘excitotoxicity’. Excitotoxicity is one of the mechanisms believed to cause motor neurones to die in MND. An overload of glutamate can cause the motor neurone to be constantly ‘open’, leading to an excess build up of calcium within the cell. This build up of calcium eventually causes the motor neurones to die. Stopping this glutamate overload is key to Helena’s research.
Stopping excitoxicity (Helena’s project)
The glutamate receptor normally prevents calcium entry, enabling the cell to control this process. When cells make a receptor, the information coded in the DNA is put into an RNA molecule, which acts as a messenger carrying the information from the nucleus to the rest of the cell. The cell usually edits this RNA molecule before it is used to create the glutamate receptor. However, this RNA editing process appears to be disrupted in MND, and so the glutamate receptor becomes faulty and is unable to control the amount of calcium entering the cell, leading to cell death.
During the first two years of Helena’s research, she has been focussed on this RNA editing process, and how it can be improved in MND. One way is to improve the cell’s editing machinery. By manipulating the enzyme that carries out the RNA editing, the number of “edited” glutamate receptors could be increased. Helena has also been working on purposefully disrupting the RNA editing to observe any other effects in cells.
Antisense
The way in which Helena has corrected this process is by using antisense oligonucleotides. This is a new type of therapy that is designed to bind directly to the faulty RNA target sequence and correct it. By correcting at this early stage, before the faulty glutamate receptor is produced, Helena hopes to reduce excitotoxicity from happening within the cell, and so reducing the calcium levels and stopping the motor neurone from dying.
Next steps?
Helena said: “The next steps in my project are to move my treatments from the cell lines that I’ve been working in to neuronal cells. I can then assess whether my antisense therapy can improve RNA editing enough to prevent neurones from dying.”
The ability to improve RNA editing gives this research a foundation to build on in order to develop a potential treatment for MND.

More about this research
Dr Philip Chen, Prof George Dickson and Dr Linda Popplewell, based at the Royal Holloway, University of London, were awarded £88,924 in 2012 for Helena’s three year PhD studentship.
This project aims to investigate whether small strands of DNA, known as ‘antisense oligonucleotides’ can be used to improve the efficiency of the RNA editing process, resulting in more properly formed glutamate receptor proteins and making the neurone more resistant to damage.
Read more about this and other research projects funded by the association here.
A great lay person explanation to the glutamate PhD. Can’t wait to hear further.
Good progress,fingers crossed everyone for this one.
Need to speak to this lady
I am looking forward
I was wondering if this would work
On Stiffperson syndrome?
Hi Ann,
Stiff person syndrome (SPS) is an autoimmune disease – a condition where our immune system begins to attack glutamic acid decarboxylase (GAD), which is involved in nerve transmission. Due to this disease process being different to MND it is unlikely this technique will work.
As it is the immune system which is attacking the nerve signalling process in SPS, treatments need to target and dampen the immune response as this is what is at fault. Changing the glutamate receptor from the faulty MND protein to a healthy one in Helena’s project will not change the immune system reacting to GAD in SPS, as this has not been changed and it is the immune system at fault and not the GAD itself.
I hope this helps answer your question but if you have any further queries please do not hesitate to email us on research@mndassociation.org.
Kindest regards,
Samantha
MND Association, UK
This antisense treatment targets the
How is the difference between the two, MND and SPS, determined. What markers indicate that my son has MND and not SPS.
Hi Chris,
As SPS is an autoimmune disease against glutamic acid decarboxylase (GAD) – this means our immune system is producing antibodies against this enzyme. Therefore, a blood test can measure the levels of GAD antibodies in the blood, if these are elevated then it can indicate SPS whereas in MND these antibodies are not elevated.
I hope this helps answer your questions, but if you have any further queries please do not hesitate to contact us on 01604 611 880 or research@mndassociation.org.
Kind regards,
Samantha
MND Association, UK
Thank you
Helena Chaytow – is there any news regarding your research. My son passed away on 20th February so I am now continuing my endeavours to prove a causal link between my sons MND and his use of Protein shakes advertised as being high in glutamate. My dialogue has been with SKB who though at first were co-operative eventually stopped responding. I have been extremely busy caring for my son over the last two years and so couldn’t continue my campaign. I am now able to renew my efforts and hope that some progress has been made through research to show a link.
Thank you for your comment.
Helena has now finished her PhD study and is writing up her thesis. To add to what is written above, I understand that the researchers involved may continue to study the glutamate receptor and how they can improve the efficiency of the faulty RNA editing process and ensure the receptor functions normally.
As far as I am aware, no link has been proven between protein shakes and MND. MND is a complex disease and we do not fully understand what causes it, though it is likely that it is the combination of several factors – some genetic, others to do with environment and lifestyle – that cause the disease to develop. this combination is not the same for every person. So even if a link between protein shakes and MND was proven, it is unlikely it would be the sole explanation for your son’s MND.
Please email us on research@mndassociation.org if you have more questions.
Kind regards
Sara
MND Association, UK