Despite the winter chill, there is a warm fuzzy feeling today with the news of a paper published in the journal ‘Brain’ by an MND Association funded Research Fellow, Dr Scott Allen. Based at the Sheffield Institute for Translational Neuroscience (SITraN), Dr Allen was awarded a Senior Non-Clinical Research Fellowship by the Association in 2016, and we are immensely proud to have been able to play a supporting role in his work.

In his paper, Dr Allen and his colleagues took a novel approach to understanding how MND affects the pathways that are important for making energy in cells of the central nervous system (CNS), that are crucial to keep motor neurons functioning and alive. Specifically, his work has pinpointed a specific mechanism that is changed in MND. The team also demonstrated that there is the potential to tackle this issue by circumventing the problem in order to maintain a critical energy balance in the CNS, and therefore potentially identifying a significant new target in the development of future treatment.
Changes in energy metabolism in MND
Generally, people with MND are advised to try to maintain their calorie intake as the disease is ‘energy hungry’. Simply put, it appears that in people with MND something happens that makes people with MND burn more energy through an increased rate of their metabolism (the process of converting food into energy).
Understanding and combatting the changes in metabolism at the cellular level has been considered important and a potential target for therapeutics, but, to date, very little is known about how precisely these changes occur in people with MND. It has long been thought that if we can understand the biology behind this change in metabolism, there could be a potential for a targeted therapy to slow or even stop the rate of disease progression. In partnership with people with MND, Dr Allen has made a significant step towards understanding a component of this change in metabolism.
Problematic support cells
In order to make this research possible, Dr Allen used skin cells generously provided by people with MND , which were then reprogrammed (changed) into cells called ‘astrocytes’ using a method developed by Dr Laura Ferraiuolo and Dr Kathryn Meyer. Astrocytes are star-shaped cells found in the brain and spinal cord, that are essential to maintaining the health of motor neurons. Like dedicated valets servicing every need of the highly demanding master, these specialised cells play a key role in supporting neurons by acting as their crucial source of energy. It is thought that if MND causes changes in astrocytes, this could lead to the death of motor neurons as these vital caretaker cells are no longer able to provide the correct support. However, as yet, no one has been able to identify exactly what is happening to cause the problems in MND.
To tackle this, the team worked with a biotech company Biolog, Inc., a world leader in cell analysis, to develop an ingenious method that combined several advanced technologies to perform ‘metabolic scanning’. This allows them to look for and find differences between the metabolism of cells from people with MND and healthy controls (cells from people without the disease). Using this technique, the team looked at how 91 different substrates (cellular foods) are used by the cells to identify which, if any, of these are not used properly in people with MND.
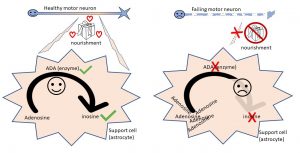
The team found that astrocytes from people with MND had a disruption in a particular cellular pathway that is solely responsible for changing a chemical ‘adenosine’ to another called ‘inosine’. This change is critical for the correct energy manufacture. In cells this conversion is controlled by an enzyme called adenosine deaminase (ADA), which was found to be reduced in the astrocytes of people with MND. Importantly, this was also found to be the case in both people with familial and sporadic MND. This is a highly significant finding as it may mean that a common mechanism of action is at play in the majority of MND cases and a single treatment could therefore be applied to all people with the disease.
To thoroughly and rigorously test their findings and confirm that they had found a genuine mechanism, Dr Allen and his team performed two further experiments. Firstly, they directly increased the amounts of adenosine in both the control cells and cells from people with MND, and found its increase was toxic in all cells, although the MND cells were more sensitive. This showed that the accumulation of adenosine that happens as a result of the loss of efficient ADA enzyme has the potential to damage neurons.
In a second test Dr Allen then caused an increase in adenosine in the control cells by preventing the enzyme (ADA) from working. (This was done by adding a chemical which specifically stops ADA from functioning). Without ADA working, adenosine began to accumulate and increased motor neuron death. This toxicity looked similar to what was seen in the cells from people with MND, suggesting the relevant mechanism, lack of ADA enzyme causing the reduction in inosine production from adenosine, has been identified.
The work of Dr Allen and colleagues has shown that there is a ‘road block’ in the pathway that converts adenosine to inosine. It therefore makes sense to see if ‘going around’ this blockage could restore normal function and prevent the death of neurons. In theory, this could be tested in a number of ways by trying to either (1) reduce the build-up of adenosine, (2) increase the amount of adenosine converted to inosine by boosting the ADA enzyme, or (3) adding inosine to trick the cells into carrying on as normal as if the pathway is working as it should.
To test this, Dr Allen fed the astrocytes inosine, which was able to bypass the effect caused by the lack of ADA enzyme and this had a positive effect on the energy of the cells. Inosine supplementation in the lab dish increased the astrocytes’ energy levels and they became more supportive towards motor neurons, resulting in an increase in motor neuron survival. By increasing ADA levels, combined with inosine supplementation, this could be a potential therapeutic approach to test in people with MND.
Can these findings result in a treatment?
Although this work has not produced an effective MND treatment yet, these are important findings as this is the first time a specific component of the energy pathway and its parts have been pinpointed. These components and mechanisms can now be targeted and add to our understanding of the biology of MND, and may form the foundation of a targeted treatment to restore the damaged energy balance in cells of the nervous system in MND.
The importance of collaboration
It is clear from this work that there is a fruitful collaboration and cooperation between MND research scientists and the added strength that comes from working together is evident. It is fabulous to see our MND centres combining and contributing together to bring about this success. Dr Allen says ”The MND Association have enabled me through their network and conferences, to set up ongoing collaborations with leading researchers in the MND field. Both Professor Martin Turner in Oxford and Professor Hector Keun at Imperial College London and their colleagues’ input and advice were crucial to this work and in enabling the Brain paper to be published and I am looking forward to working with them closely in the future”.
Patient partnerships
This work demonstrates how the generous contribution of people with MND, their families, supporters and carers are so fundamental to research. The skin samples of people with MND and controls were so vital to this work, as was the generosity of those who have supported the MND Association. It is only with these partnerships that the development of cutting edge techniques and leaps forward will happen, bringing us closer to our vision of a world free from MND.

But what actually happens next that will effect a treatment!
Hi,
Thank you for your comment.
The next step is to conduct a Phase 2/3 clinical trial with a large number of people to see whether this treatment is effective. If it would be found to be effective, approval would be sought from licensing agencies by countries worldwide.
You can find more about the trial here.
Best Wishes,
Research Development Team
MND Association
Another nail in the coffin of MND together we will beat it I am a MND patient and gave some of my skin and tissue about 4 years ago it’s great to see that all the hard work by research staff particularly at sitran starting to pay off I myself am on a ground breaking trial that appears to be helping a little so hats off to all the Sitran team also the Sheffield Hallamshire staff a particular mention to Dr Jonathon Cooper Knock and all the associated nurses and doctors who give me my monthly treatments ,where would I be without them.
Les, will you share the trial you are participating in, and what benefits you are feeling?
Fantastic work ,we all hope for a cure one day soon,as I have all ready lost my Dad his sister and brother (my aunt and uncle )and we think my grandfather,and my daughter in laws mother and my daughter in laws brother has just been diagnosed with MND at age 52 so keep up the wonderful work I can’t thank you all enough with what you are doing.