Last Thursday marked an exciting milestone in the search for effective therapies for MND as full results from the early-phase 1/2 trial of Biogen’s tofersen antisense oligonucleotide therapy for SOD1-ALS were published in The New England Journal of Medicine. In the same issue, a study investigating the use of microRNA in a viral vector to silence the SOD1 gene in two patients was also reported on.
Making sense of antisense…
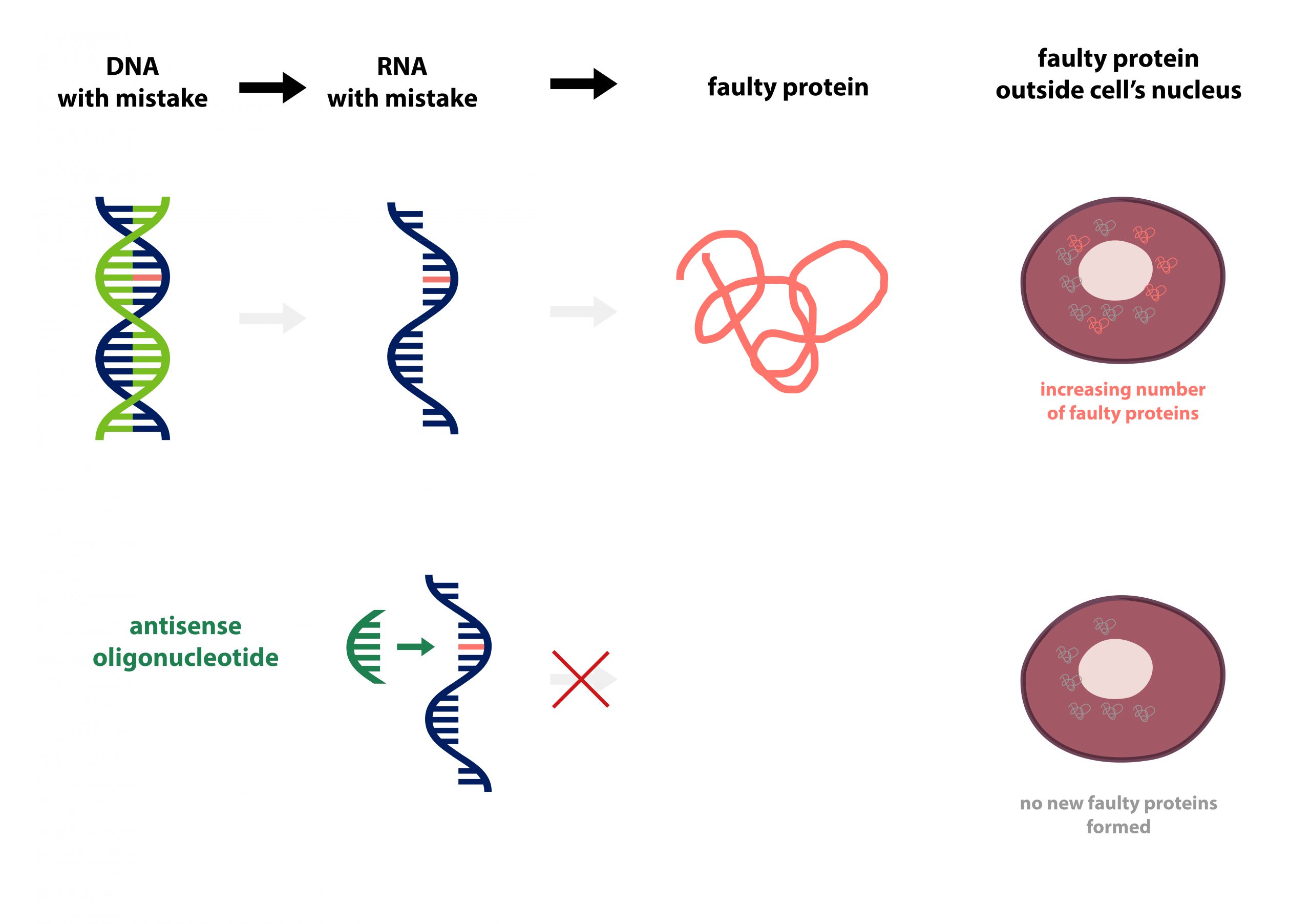
Most drugs have their effect through acting on proteins, the basic building blocks of every cell in our body, but new ‘genomic medicine’ approaches are directed at the genetic instructions for each protein. In this case, tofersen is being investigated to target the mutated SOD1 gene, which causes the second most common inherited form of MND and approximately 2% of all MND cases. These patients produce a faulty SOD1 protein that misfolds in nerve cells in the brain and spinal cord, causing a loss of control over muscles.
Tofersen is an antisense oligonucleotide (ASO) being developed by the pharmaceutical company Biogen to suppress the level of faulty disease-causing protein being produced, read more in our previous blog here. The drug is administered intrathecally into patients which means it is injected into the cerebrospinal fluid (CSF, that surrounds the brain and spinal cord), also known as lumbar puncture. Here, the Phase 1/2 study results demonstrated proof-of-concept and proof-of-biology of tofersen and is now currently being investigated in the ongoing Phase 3 VALOR study to explore the effects in a greater number of participants.
Phase 1/2 results of tofersen
As this was an early phase randomised, placebo-controlled, single- and multiple-ascending dose study, the focus was on determining the safety and dose of the drug. 48 patients were randomly assigned to receive one of four ascending doses of tofersen (20, 40, 60, or 100 mg) or placebo/dummy drug for 12 weeks. The most commonly reported adverse events in people who received one or more doses of tofersen (38 patients) were headache, procedural pain, post-lumbar puncture syndrome and falls.
Results found that patients taking the highest doses of tofersen (10 patients on 100mg) had the greatest reduction in SOD1 levels in the CSF (36%), compared to just 3% in the placebo group (12 patients). This indicates ‘target engagement’ (in other words, that the drug was having the desired effect of switching off the SOD1 gene).
The study also looked at some exploratory measures which demonstrated improvement in clinical measures with an observed slowing of decline in function, measured by the ALS Functional Rating Scale Revised (ALSFRS-R), as well as slow vital capacity and muscle strength compared to placebo. However, due to the small number of participants, these observations need to be taken as preliminary, as more data is required to provide evidence of this.
Patients who received tofersen also had a reduction in CSF neurofilament levels (an apparent marker of disease activity, see our blog post here) compared with placebo, which provides an indirect measure of an effect on reducing neurodegeneration. Further analysis suggested that the patients with fast-progression mutations may have had a greater decrease in CSF neurofilament levels and a lesser slope of clinical decline than those without.
What do the results mean?
In an accompanying editorial, Profs Orla Hardiman and Leonard van den Berg commented that these results must be considered tentative but if findings are confirmed in the phase 3 trial with longer follow-up, they may lead the way to the first potentially effective disease modifying therapy for some of the ALS population. Additionally, a reduction in neurofilament levels may provide a biomarker for future trials.

Overall, these results support the continued investigation of tofersen for treatment of SOD1-MND which is currently recruiting participants for the ongoing Phase 3 study, VALOR in centres across the world, including Sheffield and soon London (King’s College Hospital) in the UK. Although this treatment is only suitable for a relatively small proportion of people with MND, the hope is that this type of targeted technology could be applied to other genetic forms and, ultimately, pave the way to uncovering treatments for sporadic MND, which represents most cases. This includes the use of antisense oligonucleotides for ALS and frontotemporal dementia (FTD) associated with C9orf72, read blog post here.
“We have more work to do to deliver meaningful therapeutics for people with SOD1 ALS (and also C9 and non-genetic ALS) but it is collaborations such as these that make this task seem possible and probable.” said Toby Ferguson, Vice President and Head of the Neuromuscular Development Unit at Biogen. See Biogen’s news release.
Using microRNA to silence SOD1
Interestingly, another group of investigators (Mueller et al.) described a proof-of-concept study of a different method targeting the SOD1 gene in familial ALS, published in the same issue of The New England Journal of Medicine. This method involved the delivery of a single-dose of SOD1-targeting microRNA (molecules that function to regulate the expression of genes) embedded in a vector, called adeno-associated virus (AAV), via intrathecal treatment in two patients. Researchers believe this can effectively “turn off” toxic genes and proteins that cause disease. Post-mortem studies of tissue from one patient suggested suppression of SOD1 levels in the spinal cord which reflects its potential for treatment of ALS in patients with SOD1 mutations. However, additional work is required to establish its efficacy and to determine any adverse effects to the use of viral vectors. Find out more in this video by University of Massachusetts Medical School.
The SOD1 gene usually encodes a protein that neutralises radical oxygen molecules (by-products of normal cell processes that must be broken down regularly to avoid cell damage). Mutations in the gene can cause the SOD1 protein to misfold in nerve cells, forming a toxic build-up of these harmful molecules. This damage can lead to cell death, loss of control over muscles, and eventually MND. That’s where gene-silencing methods come in to reduce the amount of faulty SOD1 as a potential MND therapy.
For more information, we recommend the following blog posts:







Nice work team – are you planning on rolling out DNA swan testing kits to all families with direct links to MND cases so they know if they have the SOD1 gene?… best wishes and keep it up, Matt Julier
Dear Matt,
Thank you for reading and commenting on our blog post.
If there is a known or suspected familial link of MND (the disease runs in the family where a specific faulty gene has been identified), you can request genetic testing via your GP or by asking your local MND Care Centre for geneticists in your area. Although sometimes it is not possible to know with certainty if MND is familial, they should be able to provide some more advice on whether you would be eligible for testing. They would then put you in touch with a geneticist to have a few genetic counselling sessions to explore the impact genetic testing might have on you and your family as having an MND-causing gene doesn’t necessarily mean that the person will develop the disease. For this reason, genetic testing is generally conducted when the neurologist thinks there is a high chance of a positive result providing clear and useful information.
You can read more about inherited MND and genetic testing in our information sheets: www.mndassociation.org/research/information-sheets , or visit the NHS Oxford University Hospital’s website for more information on hereditary MND: www.ouh.nhs.uk/services/departments/neurosciences/neurology/mnd/support/is-mnd-hereditary.aspx
Best wishes,
Research Development Team
https://mndresearch.blog/2020/12/15/symposium-2020-results-from-the-phase-3-clinical-trial-of-nurown/?unapproved=2064&moderation-hash=7eb4ad60dabfd690450dd6a53fb97cfc#comment-2064